Robert Chelsea turned down the first face he was offered. It was a fine face, one that could have taken him off the transplant waiting list after just a couple months. But Chelsea—severely disfigured after a catastrophic car accident five years earlier—was in no hurry. He’d gotten used to tilting his head back so food and water wouldn’t fall out of his nearly lipless mouth. He knew how to respond compassionately to children who stared in shock and fear. The face, offered in May 2018, had belonged to a man with skin that was much fairer than what remained of Chelsea’s—so light that Chelsea, who is African American, couldn’t bear the thought of becoming “a totally different looking person.”
Chelsea’s doctors understood his hesitance. Face transplants in general are rare. Since the first partial one was performed in France in 2005, fewer than 50 have been completed worldwide. A new patient joining the ranks is always noteworthy, but Chelsea’s case carries even more weight than usual. Because he is the first African American to receive a full face transplant, Chelsea’s treatment is expected to have ripple effects that transcend his case. Disparities in the medical system that cause black Americans to die at higher rates than whites of so many things—like heart disease, cancer diabetes and HIV/AIDS—have also produced gaps in organ donation and transplantation. Widespread mistrust of the medical system has made many African Americans wary of tissue donation, contributing to donor shortages; in turn, only 17% of black patients awaiting an organ transplant got one in 2015, compared with about 30% of white patients.
Chelsea’s accidental role as the literal and figurative face of black organ transplantation is likely to help chip away at those disparities. “Having a visible, tangible reference, especially for African Americans … is so needed,” says Marion Shuck, president of the Association for Multicultural Affairs in Transplantation (AMAT). Sharing personal experiences publicly, Shuck says, could inspire potential donors with a clear example of a transplant’s positive impact. Though facial donation is rare, Chelsea’s story could encourage black Americans, and their families, to donate kidneys, livers or lungs, saving lives and reducing wait times across the country.
It took more than a year for Chelsea to get a second call—the one that would land him in a bed at Boston’s Brigham and Women’s Hospital, receiving a new face that was a near perfect skin-color match, and that made him both the first African American to undergo a face transplant and, at 68, the oldest recipient ever. “Morning by morning, new versions [of me] unfold,” Chelsea said on the day he was discharged from the hospital in August, nearly a month after surgery. “[But] I feel like myself.”

Chelsea was having car trouble one Monday night in August 2013, so he pulled onto the shoulder of a highway outside his home near Long Beach, Calif. Soon after, a drunk driver slammed into his car, and it burst into flames. Chelsea, a sales manager for a rubber-stamp business, was rushed to a hospital with third-degree burns covering almost half his body.
After being transferred to the University of California Irvine Medical Center, Chelsea spent four months drifting in and out of consciousness as doctors fought to save his life. He had 18 surgeries in that time—mostly skin grafting for his burns, but also abdominal operations to treat serious gastrointestinal complications that had developed as his body struggled to stay alive. Blood pressure medications shunted blood flow to his heart and away from his extremities, leading to tissue death in his lips, nose and fingers. One of his surgeons, Dr. Victor Joe, called him “one of the sickest patients we’ve had.”
Chelsea left UC Irvine in December 2013 with his life—but by the end of his recovery he would lose his lips, the end of his nose, several fingertips and two-thirds of his intestines. His face was severely scarred, and his hands were covered in cadaver skin that matched Chelsea’s skin tone but never quite mimicked its texture; Chelsea called it his “snakeskin.” All told, he would eventually carry the skin of three different people. An organ donor himself before the accident, he had no idea how difficult replacing his skin would prove to be.
The barriers went up long before Chelsea was born. In 1932, researchers from the U.S. Public Health Service launched a study at Alabama’s Tuskegee Institute that would change the American medical system for decades to come. The trial was covertly designed for researchers to observe the effects of untreated syphilis over the course of four decades. Six hundred black men, mostly share-croppers, enrolled in the trial, lured by the promise of free transportation, meals and medical care. About two-thirds of the men had syphilis, and half were given the then standard treatment of arsenic and mercury. The other infected men were given no treatment at all—even after penicillin was discovered to be an effective syphilis therapy in the 1940s. They were left to die; pass the disease on to partners and children; or develop complications like heart failure, mental instability and blindness.

When the Associated Press exposed the study in 1972, public outcry was immediate. Survivors and the families of deceased patients won roughly $10 million in a 1974 settlement. Two decades later, in 1997, President Bill Clinton apologized for Tuskegee, calling it “deeply, profoundly, morally wrong.” But the wound was deep, and it would scar. “African Americans still do not believe the health care profession will take care of them,” Shuck says.
That mistrust wasn’t built on Tuskegee alone. In the 1800s, enslaved people were commonly drafted as unwilling, unanesthetized subjects for medical experiments, and their deceased bodies were frequently dissected. Even after slavery was abolished, black patients were often turned away by white doctors and hospitals. When they did get treatment, it wasn’t always ethical. Henrietta Lacks famously had her fast-replicating, cancerous cervical tissue taken without consent in 1951; the cells eventually became a lucrative cornerstone of medical research, kick-starting a decades-long debate over informed consent and who profits from scientific advancement. Such incidents, and numerous others like them, still loom large, especially in a world where many physicians, according to one 2017 research review, implicitly favor white patients. “The whole medical system follows along with the racism that the country was built upon,” says Dr. Vanessa Grubbs, a nephrologist at the University of California, San Francisco.
Famous historical examples mix with families’ more contemporary, personal stories of mistreatment, leaving many African Americans skittish of doctors, says Dr. Damon Tweedy, an associate professor of psychiatry at the Duke University School of Medicine and the author of Black Man in a White Coat. “There’s some remnant of that that you internalize,” he says. Though he’s black himself, Tweedy says patients have asked if his hospital is “experimenting” on them or using them as “guinea pigs.”
It’s perhaps no surprise, then, that many African Americans are hesitant to volunteer for medical -studies—often an important first step in developing effective treatments. A ProPublica analysis of Food and Drug Administration data found that in many trials for drugs approved from 2015 to 2018, less than 10% of research participants were black. (The research community is working to close such gaps through initiatives like the National Institutes of Health’s All of Us trial, a million-person study trying to recruit under-researched populations.) As a result, doctors today know far more about white bodies than about black bodies, even though black Americans report higher rates of conditions like Type 2 diabetes, heart disease and many cancers—largely because of centuries of structural inequities that have, among other consequences, left more than 10% of black Americans without health insurance compared with about 6% of whites, and 21% of black households without secure access to quality food compared with less than 10% of white households.
Understanding that complicated history is crucial to understanding the state of organ transplantation in the U.S. today. Black patients, on average, face longer waits for major organs like kidneys, lungs and hearts than white patients, meaning more may die before they get the surgeries they need. That’s in part because African Americans, who make up about 13% of the U.S. population, account for roughly 30% of the transplant waiting list, according to federal data. By contrast, about 65% of deceased donors are white, and white Americans make up only about 40% of the waiting list.
Higher rates of chronic disease among African Americans mean both that a disproportionate number need transplants, and that fewer have living family members healthy enough to donate organs like kidneys and livers. Even if they do, Shuck says, “we don’t want to ask our family because we don’t want to put them at risk, so we languish longer.”
Religious and philosophical beliefs may also play a role, says Dr. Charles Bratton, a transplant surgeon at Loma Linda University Health who has studied donation disparities. Jehovah’s Witnesses, 27% of whom are black in the U.S., do not accept blood transfusions, which can also dissuade them from being involved with organ transplants. Members of some religions that believe in resurrection, like Southern Baptists, may also want their bodies to be whole when they die, even though most religions allow organ donation. Finally, people in the U.S., unlike those in some European countries, have to actively opt in to organ donation rather than opting out, further depressing donation rates. All told, according to the most recent federal survey on attitudes toward organ donation, only 39% of black Americans’ driver’s licenses marked them as organ donors, compared with almost 65% of white Americans.
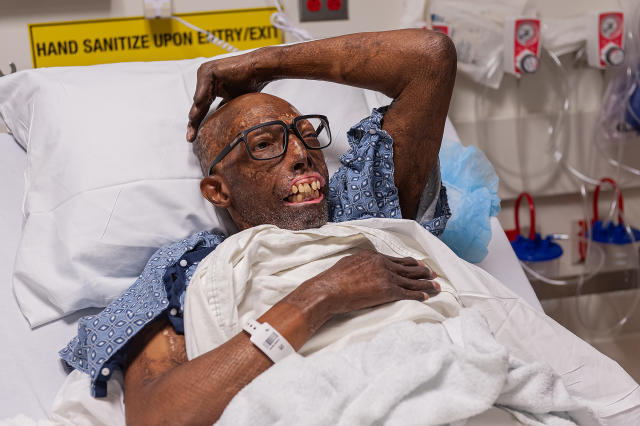
“Do you see the way they look at me? It’s cute. They’re curious,” Chelsea said the first time we met, in November 2018, months before his surgery. He’d told me to drive straight from the airport to his gym in Victorville, Calif.—it was Monday, and he always worked out on Mondays. From there, we went on an errand to Metro-PCS, then to pick up tacos for lunch. People stared, but Chelsea was good–natured about it. “I don’t blame them,” he said. “It’s scary. It’s like I’m wearing a Halloween mask.”
Five years after his accident, Chelsea insisted that his appearance didn’t bother him, in large part thanks to the deep-seated Christian faith that helped him through his recovery. He also joked that he was “no knockout looker” before the accident, though friends and family remember it differently. His acceptance was so unflinching, in fact, that when Dr. Bohdan Pomahac, director of plastic-surgery transplantation at Brigham Health, first approved him for a face transplant, Chelsea wasn’t sure he wanted one at all.
Chelsea’s attitude was exceptional. Losing one’s face—a person’s introduction to the world—is psychologically scarring for most who experience it. Face-transplant recipients are required to undergo extensive counseling to ensure they’re prepared to accept their new appearance. It can be especially difficult when one’s racial identity is also at stake. While a black patient awaiting a kidney or heart doesn’t need a black donor, a complexion match is considered crucial for visible transplants, to preserve as much of one’s identity as possible.
Physical appearance is far from the only determinant of racial identity, but it’s certainly a factor, says Jessica DeCuir-Gunby, a professor at North Carolina State University who studies the topic but has not worked with Chelsea. Accepting a face from a donor with a much lighter skin tone could present a nuanced set of emotions, she says, since black identity exists across a spectrum of colors, hair textures and facial features. A drastic change in appearance can unmoor someone from his or her identity, potentially resulting in psychological trauma, she says. Dr. Sheila Jowsey-Gregoire, a transplant psychiatrist at the Mayo Clinic who has not worked with Chelsea, says that while most face-transplant patients have done the hard work of accepting that they’ll never look exactly like they once did, altering their racial identity could lead to unforeseen negative consequences.
The need for a precise color match further shrinks an already small pool of potential donors: in the federal survey on organ donation, only about 41% of black respondents said they’d be at least “somewhat” willing to donate a face, vs. about 61% of Caucasian respondents. Even Chelsea, who is largely un-interested in the superficial aspects of appearance, balked at the prospect of accepting a face so much lighter than the one he knew.
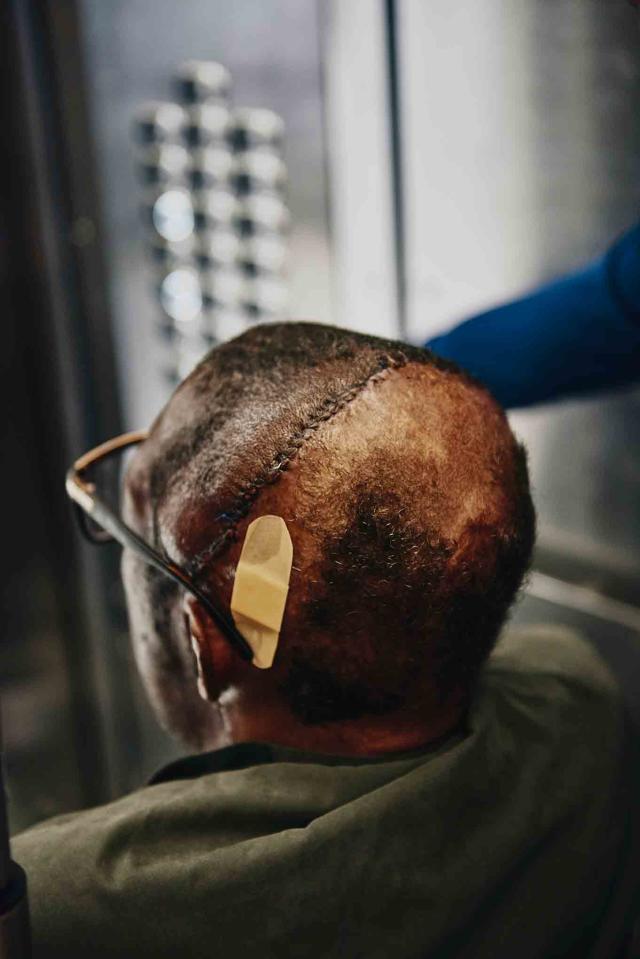
It wasn’t just the possibility of a stranger in the mirror that gave Chelsea pause. Organ-transplant patients need to take immune-system suppression drugs for the rest of their lives to keep their bodies from rejecting their donor organs. His health had been stable in the years after his recovery from the accident, and the transplant would take him back to a world of constant doctor’s appointments and medications. And while Chelsea’s surgery would be performed for free, thanks to a grant Brigham and Women’s received from the Department of Defense to test a less cumbersome post-transplant immune-suppression regimen, his family would still have to pay some travel and caretaker expenses associated with the surgery. When NYU Langone last year performed the first face-transplant covered by commercial insurance, the hospital estimated it would have cost about $1.5 million out of pocket. Even without taking on any of those costs, Chelsea’s family had to launch a GoFundMe to pay for miscellaneous expenses, raising more than $75,000. Even more conventional transplants can be expensive. Tweedy says the financial burden of becoming a living donor and recovering from an invasive surgery, which often requires time off from work, discourages lower-income patients—who tend to be disproportionately of color—from participating in transplants.
Chelsea’s 30-year-old daughter Ebony was even more concerned than her father. Seeing him in critical condition after his accident was like “going to a movie theater and watching the scariest movie that they had out, and you replayed it over and over and over,” she says. “You went through all that, and all of a sudden you want to go over here and [have another procedure]? Any surgery has complications.”
But Chelsea ultimately wanted to eat and drink normally, to spit, to swallow a pill, to close his mouth—and, most of all, he said, to kiss Ebony on the cheek. Eventually he decided those promises outweighed the risks.
It took a while, he says, to recognize the significance of becoming the first African-American face transplant recipient. When the realization came, it was tinged with discomfort. “There is a degree of pride, admittedly, and yet I’m not sure that it’s something to be proud of,” Chelsea said about six months before his surgery. “To celebrate an individual because they haven’t done anything any more than anybody else, they just happened to be there at the right time … there’s nothing holy about those actions.” Still, Chelsea could recognize that the surgery came with a higher purpose: providing a positive example of how transplantation can change lives, especially for black Americans. “We are a lot more hesitant to be a donor,” he says. “It causes us to lose out when we need a kidney or a liver or a lung.”
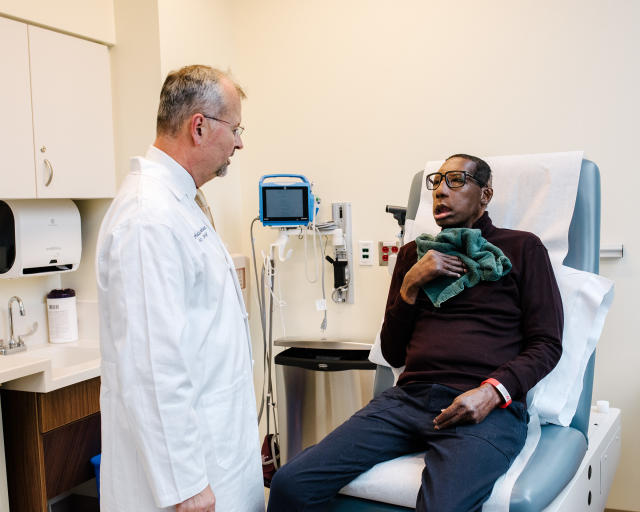
Chelsea’s surgeon was undaunted by the year-plus search for a donor, even after coming so close with the first face last spring. “All it takes is one. Sooner or later you will find one,” Pomahac said about six months before ultimately finding the donor face that would become Chelsea’s. Last year, less than 7% of the organs procured in overwhelmingly white New England, where Brigham and Women’s is located, came from African-American donors. While Pomahac and his team could theoretically accept a donor organ from any region, the hospital’s policy dictates that travel to the donor site cannot exceed four hours, in part to preserve the function of the organ. To look outside New England—as Pomahac and his team eventually did—would require finding a location within easy flying distance of Boston.
Chelsea never second-guessed his decision to turn down that first face—but he also couldn’t have guessed how long the search would drag on. He and Pomahac had used a 1-to-18 scale to discuss potential donors’ complexions—1 being the lightest—on which Pomahac says Chelsea is a 15 or 16. They originally looked for donors falling from 8 to 16 but, after months of no luck, Chelsea eventually agreed to consider donors as light as 5. Even that didn’t work.
Then, this spring, Pomahac encouraged Chelsea to consider a full facial transplant instead of the partial one they’d planned to replace just the lower portion of his face. Pomahac was mostly focused on cosmetics, but Chelsea and his family hoped the decision would also speed up the search process by eliminating the need to blend exactly with Chelsea’s surviving skin, making imperfect matches less obvious. Chelsea agreed to the full transplant—and finally, more than a year after he joined the transplant waiting list, he got the call in July. His doctors had found a match with a near identical skin tone. He had 24 hours to make the biggest decision of his life, based only on descriptions of the donor’s complexion, age and medical risk factors, then fly from Los Angeles to Boston for the surgery. “I had to believe,” he said that day. “I was just hoping that it was a legit call.”
In another state, another man had just received a very different phone call. Shortly after learning that his 62-year-old brother had died suddenly, James, 51, was approached by the Gift of Life Donor Program about donating his brother Adrian’s internal organs—and his face. James didn’t know his brother’s wishes but was staunchly in favor of organ donation himself after serving in the Air Force, where he says the practice was valued. He knew that Adrian—a talented athlete and guitarist who loved to play Hendrix, worked in construction and was always “ready to light up a room”—would want to help someone else. “He would give the shirt off his back for anybody,” James says. After calls to his five other siblings, James decided to move forward with donation, comforted by the fact that part of his older brother would be “still here and on this earth, [so] he lives on.” He had no idea that his brother’s would be the first African-American face ever to be transplanted.
To Chelsea, the face he would receive was anonymous. But the loss another family had to suffer to give him a new beginning was the only subject that made him grow somber in the chaotic hours before surgery.
“Losing a loved one and being asked something like this … I can’t imagine,” he said. “I do feel hopeful that I can pick up some of the pieces that the family may have lost.”

Those 24 hours began a well-rehearsed dance of more than 45 surgeons, anesthesiologists, nurses, pharmacists, research fellows, social workers and a chaplain. Pomahac, who with his team had performed eight previous face transplants, boarded a plane with three other doctors to get Adrian’s face, which they carefully removed and placed on ice. In Boston, the Brigham and Women’s staff prepped Chelsea for surgery, exposing the nerves and vessels that would soon be attached to the donor’s tissues using hair-thin sutures so tiny that Pomahac had to sew them under a microscope.
When Chelsea emerged from the 16-hour surgery, his godson, Everick Brown, could focus on only one thing. “I was like, ‘Look at those juicy lips,’” Brown laughed. “‘He’s going to be happy.’” Even in the early hours of Chelsea’s recovery, before the swelling had gone down, Brown could tell Pomahac and his team had done a good job. Aside from his lips, Brown said, his godfather looked shockingly similar to the way he did before. “It was a joy,” Brown said. “It’s the first time I’ve used the word miracle.”
By the second day post-op, Chelsea’s heaviest pain medication was Tylenol. Within 10 days, he was eating, talking and breathing on his own—and though Pomahac says the nerve-rich lips never regain full function after a transplant, Chelsea’s dream of kissing his daughter on the cheek is within reach.
It’s not only Chelsea’s life that will change. Tweedy says stories like his can help rebuild trust with the medical system. “Sharing,” he says, “can go a long way to healing.” Research bears that out: a 2013 study on encouraging organ donation found that successful approaches typically “comprise a strong interpersonal element that focused on the particular population’s concerns, delivered by members of the local community.” A number of awareness days and weeks—including National Minority Donor Awareness Week in August—are meant to boost donation rates, as are initiatives like the United Network for Organ Sharing’s ambassador program, which encourages donors, recipients and those on the waiting list to speak publicly about their experiences. James recently decided to take on the role informally, after learning of the historical significance of his brother’s donation. “I think it’d be a dis-service to stay anonymous,” he says.“Hopefully this story can put that in a light for others to donate.” Changes meant to bring medical equality are also taking root more broadly. A growing number of medical schools, for example, are waiving tuition to attract a more diverse pool of doctors in training, among other goals.
Before his surgery, Chelsea began establishing Donor’s Dream, a nonprofit meant to encourage and provide information about organ donation. Even in the grueling weeks after surgery, as the swelling came down, his speech and vision improved and his new skin started to glow and sprout hair, he felt that the experience was bigger than him—one that would evolve into a future he couldn’t yet imagine.
“I was concerned about humanity way before this surgery,” he said about 10 weeks after the operation, after moving into a temporary apartment in Boston, where he would complete weeks of follow-up care. “We must help one another. That’s the way I felt, and this experience has only validated that even more.”
.ya







